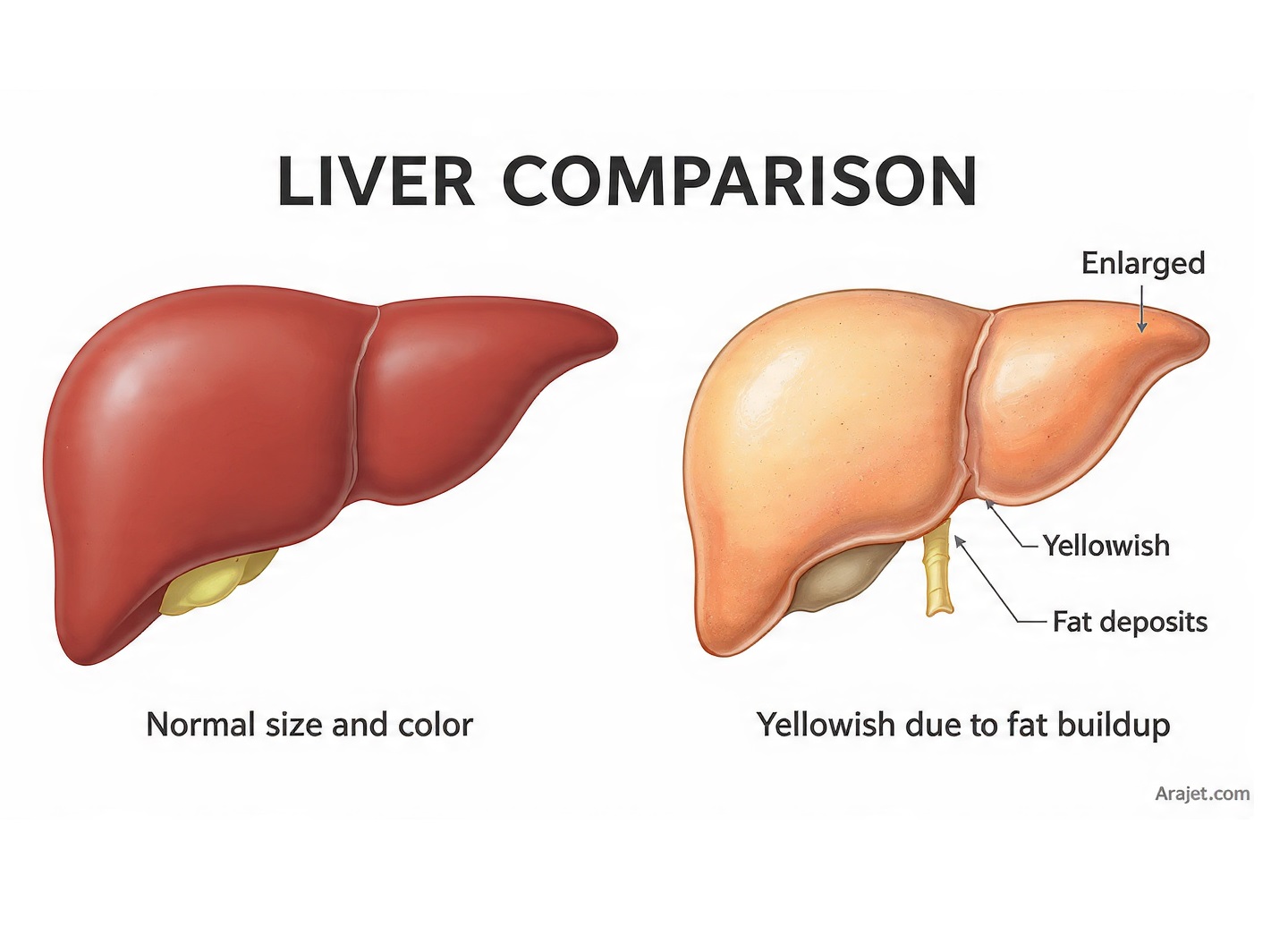
A new study flips what doctors thought about the deadliest risks for the world’s most common liver condition
If you’ve heard of fatty liver disease, you probably think of alcohol or obesity as the main culprits. But a large study from Keck Medicine of USC is forcing doctors to rethink that assumption. Researchers have pinpointed three cardiometabolic conditions that now appear to drive death risk in people with metabolic dysfunction-associated steatotic liver disease (MASLD) more than anything else: high blood pressure, pre-diabetes or Type 2 diabetes, and low HDL cholesterol.
The findings matter because MASLD isn’t rare. It affects more than one-third of the global population, making it the world’s most common chronic liver disease. And while the condition often starts silently with fat buildup in the liver, it can progress to fibrosis, cirrhosis, liver failure, and even heart and kidney disease. The new research shows that among the five cardiometabolic risk factors usually linked to MASLD — obesity, Type 2 diabetes, high blood pressure, high blood sugar, and low HDL cholesterol — three stand out as the deadliest.

What the study found
The study, published in Clinical Gastroenterology and Hepatology, analyzed data from the National Health and Nutrition Examination Survey covering US adults from 1988 to 2018. Out of 134,515 participants aged 20 and older, about 21,000 met the criteria for MASLD. Researchers then tracked all-cause mortality and looked at which risk factors predicted death most strongly.
The results were clear. Among people with MASLD:
- High blood pressure increased the risk of death by 40%
- Pre-diabetes or Type 2 diabetes increased risk by 25%
- Low HDL cholesterol, often called “good” cholesterol, increased risk by 15%
These associations held regardless of age, gender, race, ethnicity, or how many other risk factors a person had. In other words, having high blood pressure alone was enough to significantly raise mortality risk for someone with fatty liver disease.
The finding about blood pressure surprised researchers most. “Until now, it was commonly thought that diabetes was the most pressing health problem for MASLD patients, which is a key insight,” said lead author Dr. Matthew Dukewich. Senior author Dr. Norah A. Terrault added that the study helps doctors know where to focus treatment efforts.
Why this matters now

MASLD has been on the rise for decades, tracking closely with the global increases in obesity, Type 2 diabetes, and poor metabolic health. Sedentary lifestyles and diets heavy in ultra-processed, high-salt, fatty, and sugary foods are driving the condition, particularly among younger people. Cardiometabolic health has been worsening fastest in those under 35.
That matters because MASLD doesn’t exist in isolation. The same metabolic dysfunction that damages the liver also stresses the heart, blood vessels, and kidneys. Each additional cardiometabolic risk factor a patient has increases their risk of death by about 15%. Obesity remains the most common risk factor, and higher BMI is directly linked to higher mortality risk. But the new study suggests that controlling blood pressure, blood sugar, and HDL cholesterol may have an outsized impact on survival.
The liver-heart connection
The link between liver disease and cardiovascular risk isn’t new, but the strength of the blood pressure connection is. High blood pressure damages blood vessels throughout the body, including the small vessels in the liver. When combined with fat buildup in the liver, it accelerates inflammation and scarring. Type 2 diabetes drives insulin resistance and increases fatty load in the liver, worsening inflammation and injury. Low HDL cholesterol reflects poor lipid metabolism, which both contributes to fat accumulation in the liver and increases cardiovascular risk.
Together, these three conditions form a dangerous triad. People with diabetes already face roughly double the risk of serious liver disease compared to those without diabetes. When hypertension and low HDL are added to the mix, the risk compounds.
Who’s most at risk
The study found that the risk profile holds across groups. It didn’t matter whether patients were male or female, younger or older, or from different racial or ethnic backgrounds. That suggests the findings apply broadly, not just to one subset of patients.
However, certain groups may be at higher baseline risk. Heavy drinkers with diabetes, high blood pressure, or a large waist circumference are up to 2.4 times more likely to develop advanced liver disease. Alcohol consumption has risen since the COVID-19 pandemic, and it causes fat buildup in the liver just like metabolic dysfunction does. When alcohol and cardiometabolic risk overlap, the liver takes a double hit.
Mexican American youth are also disproportionately affected, partly due to a genetic mutation that increases fat storage in the liver. The prevalence of MASLD among adolescents has doubled over the past three decades, reaching almost 11% by 2008. That means more young adults are entering their 20s and 30s already carrying liver damage.
What this means for screening and treatment
For years, doctors focused heavily on diabetes management in MASLD patients. This study suggests that blood pressure control may be just as urgent, if not more so. “Knowing which aspects of MASLD might lead to poorer outcomes can help us offer patients the best possible care,” said Dr. Terrault.
Practical implications are straightforward:
- Check blood pressure routinely in anyone diagnosed with MASLD, even if they feel fine. Early treatment with lifestyle changes or medication can lower risk.
- Screen for pre-diabetes and Type 2 diabetes in all MASLD patients. Early intervention with diet, exercise, and medication can slow progression.
- Monitor lipid profiles, especially HDL cholesterol. Raising HDL through exercise, weight loss, and certain dietary patterns may help, though medication options are limited.
- Address weight and diet, since obesity remains the most common driver. Even modest weight loss of 5-10% can reduce liver fat and improve metabolic health.
Researchers also note that many patients with fatty liver disease are undiagnosed in primary care. Because the disease is often silent until advanced, some patients only get diagnosed after progressing to cirrhosis or liver cancer. That’s why experts argue for greater awareness among the public, doctors, and policymakers.
The bigger picture
MASLD sits at the intersection of two global epidemics: obesity and Type 2 diabetes. Its prevalence has risen alongside diets high in ultra-processed foods and increasingly sedentary lifestyles. Unlike alcoholic liver disease, MASLD is tied directly to metabolic health, making it a marker of broader cardiometabolic risk.
The study adds to evidence that the liver is not just a passive organ in metabolic disease. Fat accumulation in the liver interferes with glucose metabolism, increasing the risk of developing Type 2 diabetes. In turn, diabetes worsens liver inflammation and injury, creating a feedback loop that’s hard to break.
What researchers want to know next
The USC team plans further studies looking at genetics, dietary habits, and alcohol use to build more complete risk profiles. “The more we can understand about the drivers of the disease, the more we can identify those most in need of interventions and prioritize our resources for enhanced outcomes,” said Dr. Terrault.
Other research is also exploring whether all patients with Type 2 diabetes should be screened for chronic liver disease. Given that diabetes patients are more than twice as likely to develop aggressive liver disease, routine liver screening may become standard practice.
What you can do now
If you have MASLD, or risk factors for it, the message is practical rather than alarming. Focus on the things that move all three risk factors in the right direction:
- Move more: Regular aerobic exercise and resistance training lower blood pressure, improve insulin sensitivity, and raise HDL cholesterol.
- Eat for metabolic health: Cut back on ultra-processed foods, added sugars, and excess salt. Prioritize fiber, lean protein, and healthy fats.
- Lose weight if needed: Even 5-10% weight loss reduces liver fat and improves cardiometabolic markers.
- Limit alcohol: Since alcohol adds to liver fat, keeping intake low gives your liver a better chance to recover.
- Stay on top of checkups: Ask your doctor about liver function tests, blood pressure, HbA1c, and lipid panels if you have risk factors.
Bottom line
Fatty liver disease affects 1 in 5 people, and it’s no longer just a “liver problem.” The new study shows that high blood pressure, Type 2 diabetes, and low HDL cholesterol are the three conditions most strongly tied to death in MASLD patients. High blood pressure, in particular, emerged as the top threat — a shift from the previous focus on diabetes alone.
The takeaway isn’t to panic, but to pay attention. MASLD is often silent until late stages. By catching and managing these three risk factors early, patients and doctors can change the trajectory of the disease. As Dr. Terrault put it, knowing where to focus can help offer the best possible care.
References:
- Daily Mail: Scientists pinpoint three major risk factors of deadly liver disease
- EurekAlert: Three deadliest risk factors of a common liver disease identified in new study
- Keck Medicine of USC Study: Published in Clinical Gastroenterology and Hepatology